Stożek rogówki
objawy, korekcja, leczenie
Wczesna diagnoza i szybkie podjęcie leczenia to szansa na zatrzymanie rozwoju choroby
Możliwość korekcji stożka rogówki przy jednoczesnej poprawie ostrości widzenia
Najbardziej specjalistyczna diagnostyka
Innowacyjne metody leczenia

Stożek rogówki (Keratoconus) jest to postępująca choroba, w 90% przypadków dotyka obu oczu. Rogówka to przednia, wypukła część gałki ocznej. Składa się z nabłonka i śródbłonka – pomiędzy którymi umiejscowione są 2 blaszki graniczne oraz istota właściwa rogówki. W wyniku choroby rogówka staje się coraz cieńsza i przybiera stożkowaty kształt. Z powodu uwypuklenia rogówki dochodzi do zniekształcenia jej powierzchni i powstawania zaburzeń widzenia.
Pogarszająca się ostrość wzroku spowodowana jest nieregularnym astygmatyzmem, który nasila się w miarę postępu choroby. Najczęściej stożek lokalizuje się w dolnej części rogówki, poza obszarem optycznym, dlatego w początkowej fazie może nie zaburzać widzenia i tym samym być niezauważonym przez Pacjenta. Z czasem jednak w większości przypadków stożek rośnie i obejmuje tak duży obszar rogówki, że znacznie upośledza widzenie. We wczesnym stadium choroby wzrok pacjentów ulega okresowemu pogorszeniu lub poprawie (łączy się to z koniecznością częstych zmian mocy okularów).
Stożek rogówki rozwija się najczęściej przez okres ok 10 – 20 lat, po czym dochodzi do zatrzymania zmian. Jego przebieg bywa różny: u niektórych pacjentów choroba utrzymuje się w jednym stadium przez wiele lat lub na stałe, u innych rozwija się szybko lub przybiera formę okresowych pogorszeń.
W zaawansowanym stadium stożka, wybrzuszenie rogówki może prowadzić do miejscowego pęknięcia błony Descemeta powodując przeciekanie cieczy wodnistej z przedniej komory oka do warstwy rogówki. Towarzyszy temu ból, nagłe zamglenie widzenia, mlecznobiałe zabarwienie rogówki.
Nieleczony stożek rogówki może doprowadzić do konieczności przeszczepu rogówki. Odpowiednio wcześnie zdiagnozowana choroba i szybkie podjęcie terapii stwarzają szansę nie tylko na zatrzymanie rozwoju stożka, ale także na poprawę widzenia.
Objawy stożka rogówki
Stożek rogówki rośnie, ale zazwyczaj bardzo powoli. Może też zatrzymać się na dowolnym etapie: zarówno umiarkowanym, jak i poważnym. Gdy choroba postępuje, dochodzi do coraz mocniejszego wybrzuszenia rogówki. Jedynym sposobem na szybką diagnozę są regularne wizyty u doświadczonego specjalisty.


Przyczyny powstawania
Nieznane są dokładne przyczyny powstawania stożka rogówki. Istnieje natomiast kilka teorii dotyczących etiologii tej choroby. Główną przyczyną prawdopodobnie jest obciążenie genetyczne, a także wtórny efekt procesów chorobowych.
Diagnoza stożka rogówki
Podczas rutynowego badania wzroku często wczesne postacie stożka rogówki pozostają nierozpoznane. Dlatego tak ważny jest wybór dobrego specjalisty, którego gabinet wyposażony jest w specjalistyczny sprzęt umożliwiający wykonanie topografii rogówki. Nowoczesne urządzenia diagnostyczne pozwalają wykryć stożek nawet w fazie, gdy jest on jeszcze w zalążku. Taka wczesna diagnoza daje szansę Pacjentowi na szybkie podjęcie skutecznego leczenia i zahamowanie progresji choroby.
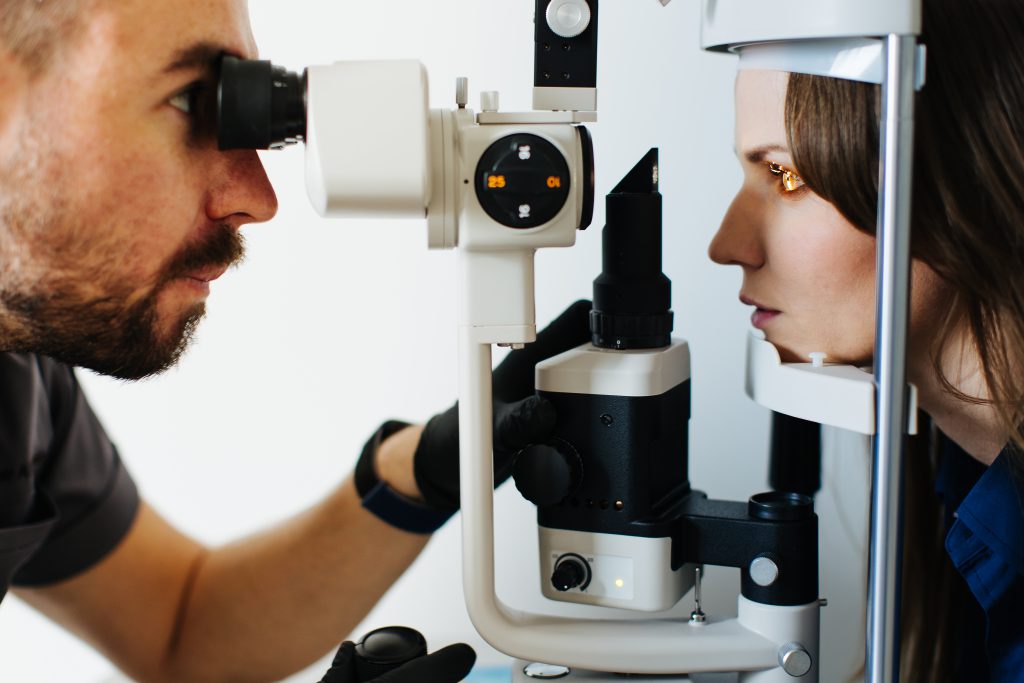

Leczenie stożka rogówki
Stożek rogówki przyczynia się powstawania astygmatyzmu nieregularnego, który istotnie wpływa na jakość widzenia. Jedynym sposobem na skorygowania wady wzroku są twarde lub hybrydowe soczewki kontaktowe, ponieważ okulary nie poprawiają widzenia. Należy jednak pamiętać, że soczewki kontaktowe nie wpływają na zahamowanie postępu choroby, lecz jedynie umożliwiają prawidłowe widzenie. Ważne jest precyzyjne dopasowanie korekcji soczewkowej, aby stożek nie był uciskany, a rogówka nie uległa podrażnieniom.

Korekta stożka rogówki
Cena badań kwalifikacyjnych
400 zł
Cena zabiegu
od 3000zł
Lekarze zajmujący się korektą stożka rogówki
Leczenie stożka rogówka – najczęściej zadawane pytania (FAQ)
Czy zabieg jest bolesny?
Zabieg korekcji stożka rogówki jest całkowicie bezbolesny. Przed przystąpieniem do zabiegu oczy Pacjenta są znieczulane specjalnymi kroplami, które eliminują możliwość pojawienia się jakiegokolwiek bólu. Podczas zabiegu możliwe jest jedynie odczuwanie lekkiego ucisku i minimalnego dyskomfortu związanego z przytrzymaniem powiek przeznaczoną do tego celu rozwórką okulistyczną.
Ile czasu trwa badanie kwalifikacyjne oraz zabieg?
Badanie kwalifikacyjne do zabiegu stożka rogówki trwa około 1,5 godziny. Natomiast zabieg Cross Linking to procedura trwająca około 60 minut.
Czy możliwe jest przeprowadzenie badania kwalifikacyjnego i zabiegu w tym samym dniu?
Ze względów bezpieczeństwa, nie zaleca się wykonywania badania i zabiegu w jednym dniu. W trakcie kwalifikacji poszerzane są źrenice które do zabiegu muszą wrócić do swojego pierwotnego kształtu. Zwykle trwa to około 6 godzin.
Czy zabieg może zostać wykonany na jednym i drugim oku jednocześnie?
Zabieg wykonywany jest zazwyczaj w odstępie kilku dni, maksymalnie tygodnia.
Czy efekt zabiegu Cross Linking jest trwały?
Zabieg Cross-linking trwale hamuję progresję stożka rogówki i pozwala na uniknięcie dalszego ścieńczenia i degeneracji powierzchownej warstwy gałki ocznej. Na pełny efekt trzeba jednak poczekać kilka miesięcy.
Jak szybko po zabiegu korekcji stożka rogówki można wrócić do normalne aktywności?
Po zabiegu stożka rogówki, należy ściśle przestrzegać zaleceń lekarza prowadzącego.
Przez pierwsze kilka tygodni, nie wskazane jest korzystanie z sauny, basenów, solarium czy nadmierna ekspozycja na słońce. Nie powinno się również wykonywać nadmiernego wysiłku fizycznego.
Czy zabieg Cross Linking jest bezpieczny?
Zabieg Cross Linking to bardzo małoinwazyjna i bezpieczna metoda korekcji stożka rogówki
Na czym polega zabieg Cross Linking?
Zabieg Cross Linking ( CXL) polega na nasyceniu rogówki ryboflawiną, czyli witaminą B12, a następnie utwardzenie jej za pomocą promieni UV. Naświetlenie rogówki ultrafioletem, powoduje powstanie kolagenowych wiązań poprzecznych w rogówce, dzięki czemu staje się ona silniejsza, sztywniejsza i mniej podatna na odkształcenia.
Czy często zdarzają się powikłania po zabiegu korekty stożka rogówki?
Zabieg korekcji stożka rogówki poprzedzają specjalistyczne badania kwalifikacyjne, dzięki czemu można wykluczyć ryzyko jakichkolwiek powikłań
Czy wada wzroku jest przeciwwskazaniem do wykonania korekty stożka rogówki?
Nie, wada wzroku nie stanowi przeciwwskazania w wykonaniu zabiegu. Co więcej po zabiegu korygującym stożek rogówki, Pacjenci zauważają poprawę ostrości widzenia.
Jak często trzeba kontrolować wzrok po zabiegu stożka rogówki?
Pacjenci ze stożkiem rogówki, powinni być pod szczególną opieką lekarza okulisty. Dlatego Po odbyciu obowiązkowych kontroli po zabiegu, Pacjent powinien zgłaszać się na okresowe badania przynajmniej raz do roku.
Czy możliwe jest całkowite wyleczenie stożka rogówki
Stożek rogówki jest schorzeniem, którego nie da się całkowicie wyleczyć, ale dzięki zastosowaniu zabiegu Cross Linking, nie tylko korygujemy stożek, a tym samym poprawiamy widzenie, ale również leczymy rogówkę oka hamując progresję zmian.
Jak się leczy stożek rogówki?
Najlepsze efekty leczenia, przynoszą metody operacyjne: Zabieg Cross-linking oraz pierścienie śródrogówkowe Intacs.
Co to są pierścienie śródrogówkowe Intacs?
To indywidualnie dobierane dla Pacjenta w zależności od parametrów rogówki pierścienie pierścienie, które wywierają nacisk na krzywiznę rogówki i spłaszczają jej powierzchnię. W ten sposób rogówka nabiera bardziej prawidłowego kształtu, a nieregularny astygmatyzm zostaje zmniejszony.
Jak wygląda zabieg wszczepienia pierścieni Intacs?
Laser wykonuje niewielkie nacięcia w rogówce, a następnie operator wprowadza pierścienie w nowoutworzone kanaliki
Jakie są pierwsze objawy stożka rogówki?
Jednymi z pierwszych odczuwalnych dla Pacjenta objawów stożka rogówki mogą być: szybko narastający astygmatyzm i krótkowzroczność w jednym oku:
– szybko postępujące rozmazanie, zniekształcenie obrazu w jednym oku
– efekt halo wokół źródła światła
– rozmywanie się obrazu
– widzenie mnogie
– pogorszenie widzenia w nocy
– nadwrażliwość na światło
Czy operują u Was dobrzy lekarze?
Pracujący w Optegrze (dawniej Vidium Medica) specjaliści cechują się bardzo indywidualnym podejściem do potrzeb pacjenta. Przede wszystkim słuchają Pacjenta i starają dopasować jak najlepsze rozwiązanie do jego oczekiwań.
Stale poszerzają swoją wiedzę i podnoszą kwalifikacje uczestnicząc w licznych zjazdach i szkoleniach krajowych i zagranicznych.




